Suicide
When someone is driven to take their own life, it is tragic and is also devastating for those around: family, friends and colleagues. Many of us have known someone close who has committed suicide. Doctors in general, and particularly anaesthetists, are recognised as being at greater risk of suicide than the general population. Recently, Dr Kate Harding, a GP whose anaesthetist husband Richard took his own life, bravely describes her experience of coming to terms with his death in two articles in The Guardian and the BMJ. The Association is concerned by Kate’s story and other reports of suicide amongst anaesthetists. We have been discussing what to do about the subject for some time and have recently convened an expert group to discuss how the Association might respond in terms of support for those affected by suicide and thinking about possible guidelines to help individuals and departments. An expert working group has been formed, and as a first step, a survey is planned for later this year that will seek anaesthetists’ experience of suicide in colleagues. Further detail of how to respond to the survey will follow in the coming months.
Dr Bawa Garba
Much has been written in recent months about the Dr Bawa Garba case since the GMC won its High Court Appeal against the independent Medical Practitioners Tribunal ruling not to erase her from the medical register. I don’t intend to revisit the genuine concerns over the possible disclosure of written reflections and the harm the GMC handling of the case has done to the medical profession’s confidence in its regulator.
My main concern about the case is the harm that the original conviction of Dr Bawa Garba for gross negligence manslaughter could have on patient safety. Medical error is recognised as the third highest cause of death behind cardiovascular disease and cancer. It is estimated than more than 250,000 people die in the US as a result of medical error, and we have no reason to believe that the proportionate numbers are any better in the UK. If we are to reduce this shocking statistic, we need to better understand medical error through striving to learn from mistakes. This requires moving from a culture of blame to one where healthcare workers readily admit their mistakes and learn from errors. If the courts are to prosecute individual clinicians for their genuine errors, how can we encourage people to own up to their mistakes?
From what I know of the circumstances around the tragic death of Jack Adcock, Dr Bawa Garba made errors in his management, but how many of us could say that we would not have made similar errors in the pressured situation she found herself when we were at a similar level of training and experience? It is likely that Jack’s death could have been avoided but it was not solely Dr Bawa Garba’s fault that he died; the failure of the hospital to provide adequate manpower and supervision, to provide a proper induction to a doctor returning from maternity leave to a new strange hospital, and failures of the IT system, all contributed to his death. Why the criminal justice system contrived to hold Dr Bawa Garba to account, and not the many hospital and system problems is unclear. One thing is certain; a court of law with its adversarial legal system is not the best place to unravel the complexities of medical error.
It is not that healthcare workers should be immune from prosecution but that we need a justice system that prosecutes malicious or reckless behaviour, not genuine errors that any one of us could make under the difficult, prevailing conditions that we often face.
Unless we get this right medical error will continue and possibly increase in the face of defensive clinical practice. We have just submitted our response to the Williams Review into gross negligence manslaughter in healthcare. You can read our response here.
What’s in a name?
What should we call ourselves: Anaesthetist or Anaesthesiologist? Worldwide, the prevailing term is Anaesthesiologist (with or without the diphthong). I used to be opposed to the term as an “Americanism” but my view is becoming eroded by the increasing number of countries adopting Anaesthesiology to differentiate physician anaesthetic providers, and to use the term Anaesthetists for non physician providers. If I were to call myself an anaesthetist in the US, people would think that I am a nurse anaesthetist. Last year the World Federation of Societies of Anaesthesiologists (WFSA) issued a position statement that made it clear that the term Anaesthesiologists referred to physician anaesthesia providers, while acknowledging that in some countries such physicians were called Anaesthetists. Those countries include the UK, Ireland, Australia and New Zealand. Now it looks like that list is becoming shorter. The Australian and New Zealand College of Anaesthetists is looking to change its name to “College of Anaesthesiologists” (read about it here) and I have heard rumours that the College Anaesthetists in Ireland is considering the same. It looks as though the UK will be the last bastion for “Anaesthetists”.
I tested the stomach for change a couple of months ago on Twitter and didn’t get a huge response but those that I did get were against change. So should we change, particularly now that we have anaesthesia delivered by PA(A)s who are non physician anaesthesia providers? Or perhaps we should just leapfrog and lead the world in becoming “Perioperative Physicians”? Mmmm…
Forthcoming events
 This week the Association is holding an International Reception to highlight some of our international work and in particular the Ugandan Fellowship scheme. A recent paper in March Anaesthesia evaluated the Ugandan Fellowship and demonstrated the success of the programme. In the last 10 years, by partnering with local professional organisations and providing modest financial scholarships to help young Ugandan doctors to train in anaesthesia in Uganda, the scheme has helped to greatly increase the numbers of physician anaesthetists in Uganda. But the evaluation demonstrated more than just improved manpower; there was also greater access to safer surgery and improved standards of patient care.
This week the Association is holding an International Reception to highlight some of our international work and in particular the Ugandan Fellowship scheme. A recent paper in March Anaesthesia evaluated the Ugandan Fellowship and demonstrated the success of the programme. In the last 10 years, by partnering with local professional organisations and providing modest financial scholarships to help young Ugandan doctors to train in anaesthesia in Uganda, the scheme has helped to greatly increase the numbers of physician anaesthetists in Uganda. But the evaluation demonstrated more than just improved manpower; there was also greater access to safer surgery and improved standards of patient care.
On Friday, 18 May, the Association’s Heritage Centre are holding an evening event “The Guinea Pig Club”, celebrating the pioneering work of Archibald McIndoe, maverick plastic surgeon during and after the Second World War. We welcome back Dr Emily Mayhew, author and military medical historian, who will be talking about the “Clubs” enduring legacy and inspiring member stories. This special “Anaesthesia Lates” coincides with the Heritage Centre’s new Brave Faces exhibition and the popular Museums at Night week. It should be a great evening.





























 I finish with the recent sad news of the passing away of J-P van Besouw, the Immediate Past President of the Royal College of Anaesthetists (RCoA). J-P was a towering figure in Anaesthesia and lead the recent modernisation of the RCoA and many of its developments including the Perioperative Medicine programme. He will be missed by many of us. In J-P’s memory, the family have designated the AAGBI’s charity –
I finish with the recent sad news of the passing away of J-P van Besouw, the Immediate Past President of the Royal College of Anaesthetists (RCoA). J-P was a towering figure in Anaesthesia and lead the recent modernisation of the RCoA and many of its developments including the Perioperative Medicine programme. He will be missed by many of us. In J-P’s memory, the family have designated the AAGBI’s charity – 
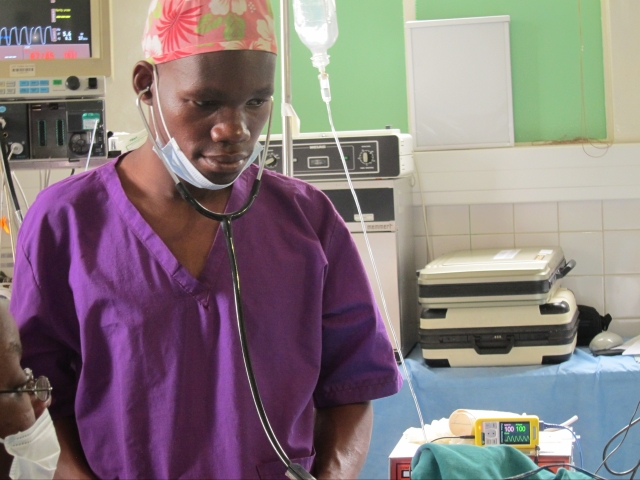 Pulse oximetry has become an essential part of monitoring in developed countries and contributes hugely to the safety of anaesthesia. However, in low income countries, pulse oximeters are scarce. The Lifebox charity has made its prime goal to ensure that patients in such countries benefit from pulse oximetry during surgery by donating oximeters and providing the training to use them effectively. A recent groundbreaking study published in Anaesthesia (read the study
Pulse oximetry has become an essential part of monitoring in developed countries and contributes hugely to the safety of anaesthesia. However, in low income countries, pulse oximeters are scarce. The Lifebox charity has made its prime goal to ensure that patients in such countries benefit from pulse oximetry during surgery by donating oximeters and providing the training to use them effectively. A recent groundbreaking study published in Anaesthesia (read the study 


